Lowering Premiums by Fixing the Market
- On average, individual premiums have increased 99 percent and family premiums have increased 140 percent in the individual market since 2013, according to shopping data from eHealth.
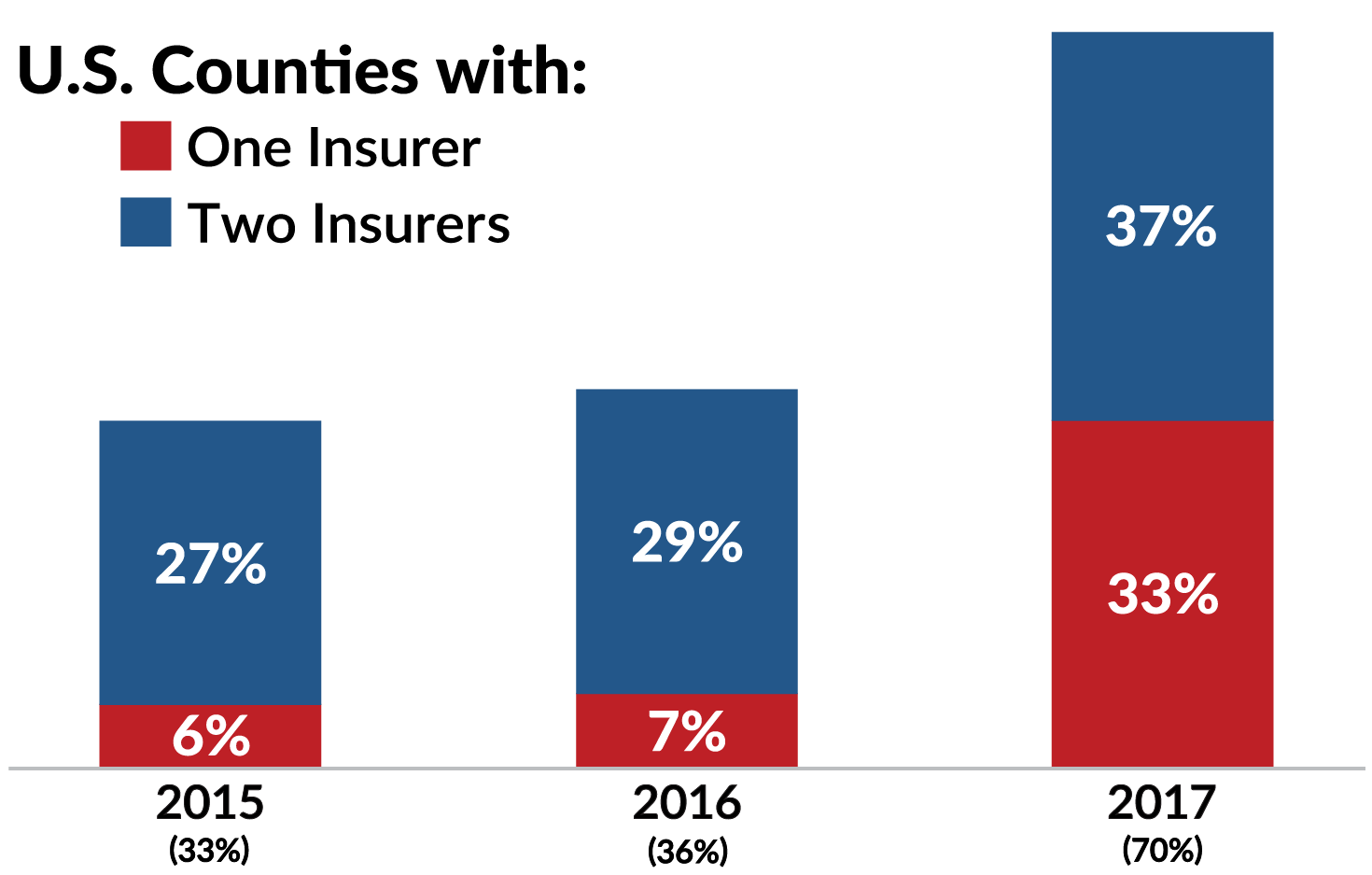
- This year, 70 percent of the nation’s counties only have one or two insurers selling coverage on the exchange.
- Republican health care reform efforts are centered on reversing Obamacare’s damage by reducing premiums, stabilizing the market, and providing relief from some of Obamacare’s mandates.
Obamacare’s health insurance regulations have increased premiums and decreased insurer competition in the individual market. Millions of Americans are stuck in this unstable market and need relief. The American Health Care Act – recently passed by the House of Representatives – includes policies aimed at reversing Obamacare’s damage.
Monopolies on the Rise
OBAMACARE’S UNWORKABLE REGULATIONS
After three years of the Obamacare system, insurance companies are largely giving up on the law’s exchanges. This year, in 70 percent of the nation’s counties, there are only one or two insurers selling coverage on the exchange. The average benchmark plan premium increase for this year was 25 percent in the 39 states relying on HealthCare.gov. According to an analysis by eHealth insurance, since 2013, average premiums in the individual market have increased by 99 percent for individuals, and family premiums have increased 140 percent.
For next year, the situation is shaping up to be even worse. Major insurers continue to leave the exchanges, including Humana and Aetna, which have both announced they are leaving all state exchanges in 2018. Other exchange insurers are requesting huge premium increases. Carefirst of Maryland requested a 58 percent price hike. Anthem has requested a 34 percent premium increase in Connecticut.
All of this is the predictable result of Obamacare’s toxic mix of unworkable regulations for the individual and small group markets.
Here are some of the law’s most onerous regulations:
| Guaranteed issue: Insurers are prohibited from denying anyone insurance coverage. |
| Essential health benefits: All insurance policies sold in the individual and small group markets must cover 10 categories of “essential health benefits.” This list mandates that many things be covered that used to be optional – some of which patients may not want or need. |
| Community rating: Insurers can only vary premiums based on an applicant’s ZIP code, age, and smoking habits, not health status. If someone waits to sign up for coverage until they are sick, an insurance company cannot charge them higher premiums. |
| Age-rating restrictions: As part of the community rating rules, the law prohibits older adults from being charged more than three times the rates for younger adults. Older adults’ health care costs are generally about five times more expensive than younger adults. This policy forced insurers to increase premiums for younger adults and slightly decrease them for older adults. A review of actuarial studies found that this Obamacare provision increased premiums for younger adults by about 33 percent. |
| Actuarial value: Insurance plans must pay at least 60 percent of a customer’s health care costs, on average. Prior to Obamacare, slightly more than half of all individual market enrollees had a plan with an actuarial value less than 60 percent. Requiring plans to cover more causes higher premiums. |
| Individual mandate: Nearly everyone must buy a Washington-approved insurance plan or pay a tax penalty to the IRS. This is meant to force people to buy insurance when they otherwise would not. It is supposed to offset the damage of the other regulations, but it has not worked very well. For 2015, more than 19 million people either paid the penalty or claimed an exemption from it. |
By mandating the standardization of all health insurance plans and controlling how insurers price their products, Obamacare has crippled the market.
ahca lowering premiums
The House bill includes many provisions aimed at lowering premiums and stabilizing the deteriorating individual market, both on and off the exchanges.
First, the bill allows Obamacare’s premium tax credits to be used to buy coverage off of the exchanges. This would immediately give consumers more insurer options. The bill also increases the credit available for younger adults to give them a greater incentive to enroll in coverage. This change is designed to improve the risk pool and help stabilize premiums.
The bill rolls back some of the Obamacare regulations that have driven up premiums. It repeals the actuarial value requirements and changes the age-rating restriction to match the normal variation of 5:1 or a ratio determined by states. This would significantly reduce premiums for younger adults.
The bill also includes a waiver that allows states to opt out of other insurance regulations mandated by Obamacare. A state could choose to opt out of the following regulations:
-
beginning in 2018, states could increase the age-rating band beyond the 5:1 ratio already adjusted by the bill;
-
beginning in 2020, states could waive the federal essential health benefits requirement and specify their own;
-
beginning with special enrollments in 2018 and for all enrollments in 2019, states could waive the 30 percent continuous coverage penalty and impose health risk rating for 12 months on people who have not maintained continuous coverage. This is only allowed if the state sets up or participates in one of the bill’s risk mitigation programs.
AHCA stabilizing the market
The AHCA also includes policies to stabilize the individual market. The bill creates a new Patient and State Stability Fund and appropriates $138 billion for the fund from 2018 to 2026. Starting in 2020, the fund would require state matching contributions, gradually reaching a 50 percent match.
A state that applies for a portion of $100 billion would be allowed to use the funds in various ways that could help stabilize the market, including:
-
Giving financial help for high-risk people to access health coverage in the individual market;
-
Providing incentives to appropriate entities to enter into arrangements with the state to help stabilize premiums in the individual market;
-
Reducing the cost of providing health insurance to high-cost users in the individual and small group markets (i.e., reinsurance, high-risk pools, risk-sharing, etc.);
-
Promoting insurer participation in the individual and small group markets;
-
Promoting access to preventive, dental, and vision services, as well as services and treatment for mental health and substance abuse disorders – inpatient and outpatient; and
-
Providing assistance to reduce out-of-pocket costs for people enrolled in health insurance.
The bill requires that $15 billion be devoted to states for maternity coverage and newborn care, as well as mental health and substance abuse disorders.
A state must apply for the funds. If a state does not apply, the administrator of the Centers for Medicare and Medicaid Services may use its allotment to pay insurers in that state for reinsurance purposes. Reinsurance provides government payments to insurers to offset some of their costs. This would decrease premiums and increase stability for insurers.
The bill requires that $8 billion between 2018 and 2023 be devoted to states that obtain a waiver from community rating. The money would be used to reduce premiums and out-of-pocket expenses for people who are charged more due to their health.
The bill also creates a Federal Invisible Risk Sharing Program within the Patient and State Stability Fund and appropriates $15 billion for it between 2018 and 2026. The program would provide payments to health insurers for claims made by eligible people. Certain health conditions determined by the CMS administrator will automatically qualify people. The administrator must determine program details such as which conditions qualify, the “attachment point,” and the coinsurance rate. Any unallocated stability funds may be used for this program as well. States may take over program operation beginning in plan year 2020.
The bill effectively repeals Obamacare’s individual mandate by changing the penalty to $0. Because the bill continues Obamacare’s guaranteed issue and community rating policies (except in states with a waiver), it includes a continuous coverage penalty to incentivize people to buy coverage before they get sick. The more people covered, the more stable the risk pool.
The Senate’s goal: FREE mArket principles
The individual health insurance market has become unstable and incredibly expensive because of Obamacare’s flawed policies and misguided regulation. The American people are waiting for relief from this failed experiment in the federal regulation of health insurance.
The American Health Care Act tries to reverse course by repealing some of Obamacare’s insurance regulations and including policies to stabilize the market. The goal in the Senate should be to fix what Obamacare broke. The law must be repealed because policies that lower premiums by fostering choice and competition cannot be layered on top of Obamacare’s faulty foundation. In replacing Obamacare, Republicans should be focused on expanding and enabling free-market principles for health reform such as allowing consumers to decide what coverage they buy, where they buy, how they buy, and with whom they buy.
Next Article Previous Article
