Key Players in the Prescription Drug Market
KEY TAKEAWAYS
- The path of a drug from manufacturer to medicine cabinet is complex, with many factors affecting the price a patient pays.
- These factors are not always publicly disclosed, hiding the true cost of prescription drugs.
- President Trump has taken steps to reform parts of the supply chain, and additional measures are starting to make their way through Congress.
The path a drug takes to its final purchaser – the patient – is complicated by many interactions along the supply chain. The participants include drug manufacturers, wholesalers, pharmacies, group purchasing organizations, and pharmaceutical benefit managers. Various transactions in the drug supply chain, including rebates, discounts, and insurance rules, make these interactions even more complex and disguise the true cost of drugs. As a result, each link in the supply chain affects access and the price a patient pays at the pharmacy counter.
In 2018, Americans spent roughly $1,000 per person on prescription drugs, about 10 percent of total U.S. health care spending.
How Pricing Dynamics Can Work in the Pharmaceutical Market
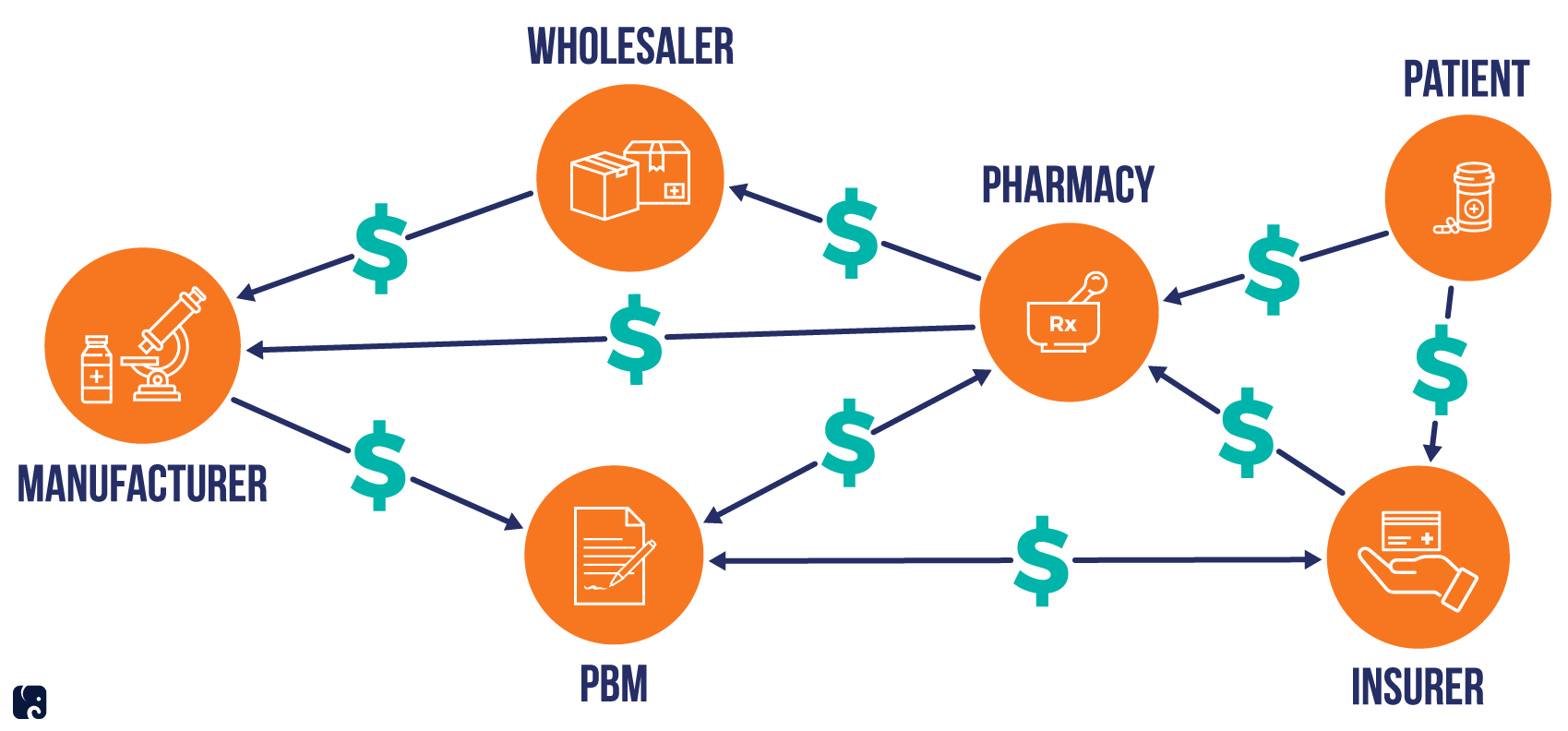
manufacturers, wholesalers, and retailers
Drug manufacturers generally distribute their products by selling to wholesalers rather than direct to consumers. A manufacturer will set a list price, known as the wholesale acquisition cost, for each drug and determine what discounts various buyers may receive. The price one wholesaler pays may be different than what another wholesaler negotiates for the same drug.
Wholesalers take physical possession of the products and then sell the drugs to pharmacies, hospitals, physician offices, and stand-alone clinics. The three largest drug wholesalers account for more than 90% of all revenues from drug distribution in the United States.
Retailers such as pharmacies mark up prices again to sell to the patient. How these markups are reflected in the patient’s payment depends on whether the patient has insurance and how his or her insurance plan is structured. Coinsurance payments will reflect any markups by wholesalers and retailers, but flat copays will not.
Drug manufacturers can offer patients discounts on behalf of insurers in the form of direct discounts, like prescription drug coupons. Patients get these discounts when they fill their prescriptions at a pharmacy.
Pharmacy benefit managers and health plans
Most patients are enrolled in an insurance plan that contracts with a pharmacy benefit manager to manage prescription drug costs. These firms – known as PBMs – negotiate with manufacturers on behalf of health plans. While PBMs influence almost every stage of the supply chain, they directly affect drug prices in two ways: negotiating drug prices for insurers; and designing the formulary – the list of drugs a plan covers. They can negotiate prices at every step of the supply chain.
A PBM will negotiate with pharmaceutical manufacturers to receive rebates. The rebate amount influences whether or not the PBM will list the drug on its formulary and in which tier of the list the drug will be placed. The location on the formulary has a great impact on the cost to the consumer. Manufacturers negotiate with PBMs to ensure their drug is placed in a good spot on the formulary so consumers do not see additional costs at the pharmacy counter. Drug manufacturers can provide rebates and other discounts based on the volume and market share worked out by the PBM and wholesaler. These rebates and discounts are not publicly disclosed.
Consumer price sensitivity
Pharmacy benefit managers and insurers influence consumer behavior by deciding how much a patient is required to pay out-of-pocket for a prescription drug. A consumer’s price sensitivity – the amount of money he or she is willing to pay – can be swayed by the insurance they have. Patients with high-deductible plans or no coverage are more likely to use fewer prescription drugs. Patients with low co-payments or coinsurance requirements are less sensitive to cost; they pay a very small portion of the true cost of the drug, making them more likely to demand high-cost prescriptions.
Insurers and PBMs also influence consumer behavior through their formularies. The list of drugs on the formulary is generally broken into tiers that have different out-of-pocket costs for patients. According to a 2018 Congressional Research Service report, formulary tiered pricing and the associated coinsurance have increased in use for more expensive specialty drugs. A consumer may pay a straight $10 co-payment for a generic drug on a formulary’s lowest-cost tier. A name-brand version of the same medication, or a different drug treating the same condition, might be on another tier and require a higher co-pay. A specialty drug could fall on the most expensive tier and require patients to pay the higher co-pay plus a 30 percent coinsurance payment.
Congressional Action
Estimating the final price a consumer will pay for a prescription drug is complicated, and the lack of transparency in the pharmaceutical supply chain only makes it harder for patients to understand. President Trump has called on Congress to address prescription drug costs. Over the past year, Senate committees have held several hearings on the subject. The Senate HELP committee is considering legislation to improve transparency in the supply chain and increase access to generic and biosimilar drugs. The Finance, Judiciary, and Aging committees have held several hearings on the subject.
Next Article Previous Article
